When you’re trying to make sense of the intersection between schizophrenia and substance use, it can feel like you’re navigating it all alone. But hope is real, and effective help is absolutely within reach in Massachusetts. This guide breaks down why these two conditions so often show up together, explores the impact of common substances, and explains how an integrated treatment plan offers the best possible chance for a lasting recovery.
Key Takeaways
- Dual Diagnosis is Common: The co-occurrence of schizophrenia and a substance use disorder is a clinical reality, not a personal failing. It's often driven by attempts to self-medicate distressing symptoms.
- Substances Worsen Symptoms: While drugs or alcohol may offer temporary relief, they ultimately intensify psychosis, interfere with medication, and increase the risk of hospitalization.
- Integrated Treatment is Essential: Treating both schizophrenia and addiction simultaneously is the gold standard of care. A unified approach that addresses both conditions at once is critical for long-term recovery.
- Local Help is Available in MA: Specialized dual diagnosis programs, like those at Paramount Recovery Centers in Massachusetts, provide the coordinated, expert care needed to manage this complex challenge and build a foundation for lasting wellness.
The Overlap Between Schizophrenia and Substance Use
To find compassionate, effective help, the first step is understanding the real story behind schizophrenia and substance use. This connection isn't about a lack of willpower or some kind of personal choice; it’s a complex clinical issue that’s deeply rooted in brain chemistry, coping mechanisms, and often, a desperate attempt to manage terrifying symptoms.
For so many, substance use starts as a way to quiet the internal chaos. It’s an attempt to find some relief from the psychosis, anxiety, or deep depression that schizophrenia can bring. This pattern of self-medication is incredibly common, but it creates a brutal cycle. The temporary escape offered by drugs or alcohol ultimately ends up making the underlying psychiatric condition much, much worse.
The reality of this overlap is a serious public health challenge. The data is stark: approximately 51.9% of adults with a serious mental illness, a category that includes schizophrenia, used illegal drugs in the last year. For a deeper dive into these numbers, you can explore the latest substance use trends on drugabusestatistics.org.

Why This Connection Matters for Families
Getting a handle on the reality of this dual diagnosis is the most important thing you can do. As you start this journey for yourself or a loved one here in Massachusetts, here are a few essential truths to hold onto.
- Co-occurrence Is Common, Not a Personal Failing: It's incredibly common for someone with schizophrenia to also develop a substance use disorder. This isn't a moral issue—it points to a real biological and psychological vulnerability.
- Self-Medication Often Worsens Symptoms: While substances might feel like a brief escape from things like paranoia or hallucinations, they almost always lead to more severe episodes down the road. This means more hospitalizations and a greater resistance to treatment over time.
- Treating Both Conditions Simultaneously Is Essential: Trying to treat the addiction without managing the schizophrenia (or the other way around) almost never works. An integrated approach that addresses both disorders at the same time is what gives someone the best shot at a real, sustainable recovery. You can learn more about the link between drug use and schizophrenia in our detailed article.
- Specialized, Compassionate Care Is Available: There is so much reason for hope. Specialized dual diagnosis treatment centers, like the ones we have right here in Massachusetts, are specifically equipped with the expertise to manage both conditions effectively.
If this is the complex challenge you or someone you love is struggling with, just taking that first step is the most powerful thing you can do. Call us today at (888) 388-8660 to speak with a caring professional who can help guide you toward the right path for recovery.
Why Dual Diagnosis Is So Common
To get a sense of the link between schizophrenia and substance use, imagine trying to quiet a blaring fire alarm with a broken volume knob. You might twist it and get a second of relief, but messing with the dial only makes the whole system more unstable. This is a lot like the "self-medication hypothesis," where someone uses substances to temporarily silence distressing symptoms like paranoia, hallucinations, or crushing anxiety. But that’s just one piece of a much larger, more complex puzzle.
The connection between these conditions isn’t a simple matter of choice or a moral failing. Instead, it’s a deeply rooted interplay of brain chemistry, genetic predispositions, and powerful environmental triggers. When you start to explore these underlying factors, it becomes clear why a dual diagnosis is so frequent—and why compassionate, specialized care isn't just helpful, but absolutely essential.
Unpacking the Reasons for Co-Occurrence
The relationship between schizophrenia and substance use isn't a straight line; it's more like a tangled web. Researchers have identified several key pathways that contribute to this high rate of co-occurrence, moving the conversation away from blame and toward a more accurate clinical understanding.
- Shared Genetic Vulnerabilities: Evidence strongly suggests that some genetic markers can make a person more susceptible to both schizophrenia and addiction. If someone carries a genetic predisposition for one, their risk for the other may also be elevated, creating a biological foundation for a dual diagnosis from the start.
- Brain Chemistry and Reward Pathways: Schizophrenia is often linked to a dysregulation in the brain's dopamine system—the same system that helps us experience pleasure and motivation. Substances like alcohol, cannabis, and stimulants hijack these very same pathways. For someone whose natural reward system is already impaired, these substances can feel especially powerful and reinforcing.
- Environmental Stressors: Life experiences matter. Traumatic events, chronic stress, and social isolation are well-known risk factors for both schizophrenia and substance use disorders. These external pressures can trigger the onset of a mental illness while also driving substance use as a way to cope, creating a vicious cycle that’s incredibly difficult to break without professional help.
The Self-Medication Hypothesis in Depth
The self-medication theory is probably the most intuitive explanation for this connection. Living with the symptoms of schizophrenia can be a frightening and deeply isolating experience. The desire to find any kind of relief is completely human and understandable.
Someone experiencing auditory hallucinations might use alcohol to try and quiet the voices. Another person struggling with the intense social anxiety and paranoia that often accompany schizophrenia might use cannabis to feel more relaxed in public. While these substances may offer a fleeting sense of control, they almost always make the underlying symptoms much worse in the long run.
This creates a dangerous feedback loop. As symptoms worsen due to substance use, the individual may use even more of the substance to cope, leading to a downward spiral of declining mental health and deepening dependency. This is a core reason why integrated treatment focused on schizophrenia substance use is so critical.
How Common Substances Impact Schizophrenia
Not all substances affect the brain the same way, and for someone managing schizophrenia, this is a critical distinction. The interaction between certain drugs and their unique brain chemistry can be incredibly dangerous, derailing treatment and making symptoms much, much worse. For families trying to help a loved one, understanding these specific risks is one of the most important first steps.
This is a practical look at how some of the most common drugs interfere with the brain and throw a wrench into recovery. While a substance might seem like it’s offering a moment of relief, the long-term consequences are often devastating. We're talking about everything from intensified psychosis to a greater chance of hospitalization. This knowledge isn’t just academic—it clarifies why getting professional help is so urgent.
The Impact of Cannabis
For years, many people saw cannabis as a relatively benign way to take the edge off anxiety. We now know that for those vulnerable to psychosis, this is far from the truth. Research has uncovered a powerful and dangerous link. THC, the main psychoactive component in cannabis, directly messes with the brain's dopamine system—the very same system that is already out of balance in schizophrenia.
This clash can trigger full-blown psychotic episodes in people who are predisposed or severely worsen the symptoms they're already living with. It's not a harmless coping mechanism; it’s a major clinical risk.
Just how serious is this? Recent studies have given us a stark picture, especially for young people. Researchers estimated that for men aged 21-30, as many as 30% of schizophrenia cases might have been prevented by simply avoiding cannabis use disorder. You can read the full research about these findings to see just how significant the connection is.
Alcohol and Stimulants: A Dangerous Combination
Alcohol is another substance people frequently use to self-medicate, often to numb the crushing anxiety and emotional pain that schizophrenia can bring. But while it might offer a fleeting sense of relaxation, alcohol is a depressant. It can drag someone deeper into hopelessness and significantly increase their risk of suicide. Just as critically, it interferes with the effectiveness of antipsychotic medications, making them less able to keep symptoms in check.
Stimulants like cocaine and amphetamines pose a different but equally serious threat. These drugs do the opposite of a depressant—they flood the brain with dopamine. This can directly kickstart or amplify psychotic symptoms like paranoia and hallucinations. The "high" from stimulants so closely mimics many of the positive symptoms of schizophrenia that it becomes incredibly difficult for clinicians to tell what’s caused by the drug and what’s a worsening of the illness itself.
This diagram helps illustrate the tangled web behind a dual diagnosis, showing how genetics, environmental stress, and the impulse to self-medicate all feed into one another.
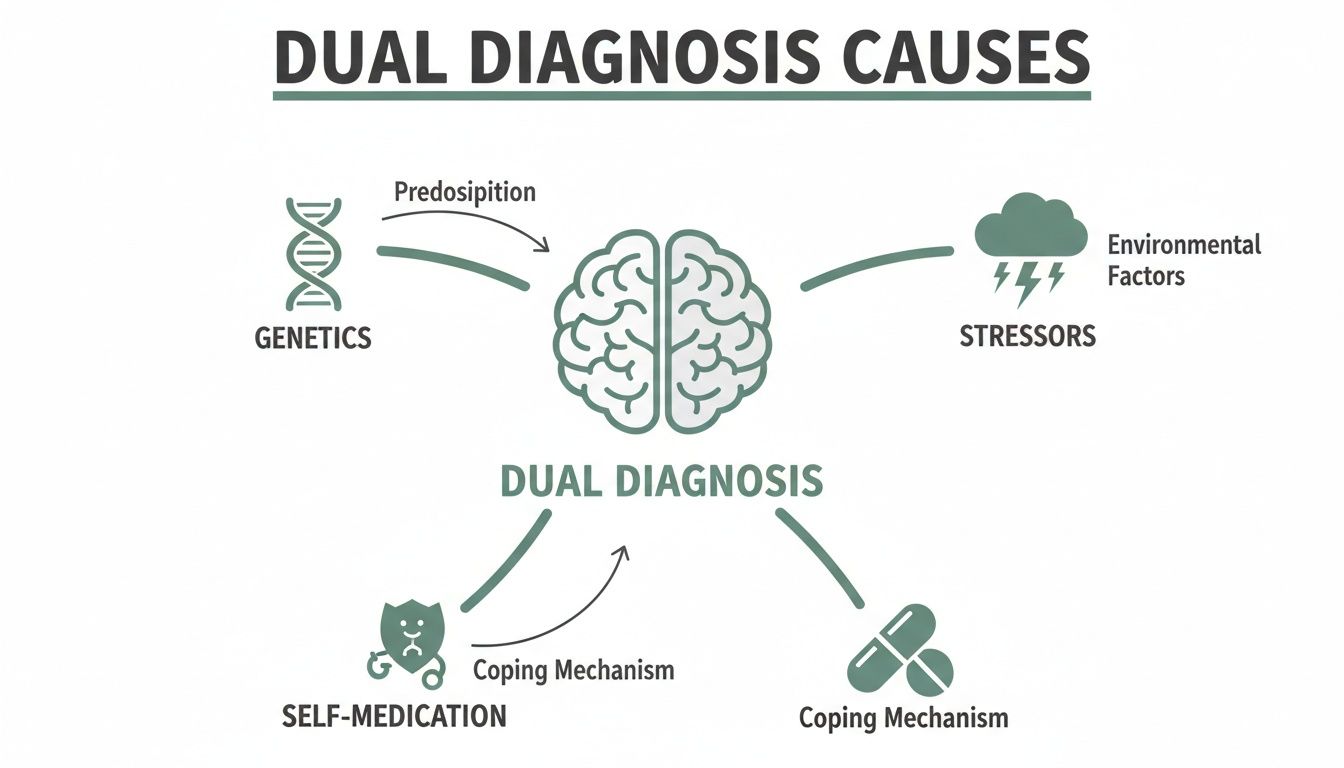
As the visual shows, schizophrenia and substance use aren't driven by a single cause. It’s a complex mix of biological vulnerability and the behavioral patterns people fall into to cope with immense stress.
For a family here in Massachusetts watching a loved one cycle between stability and crisis, knowing these substance-specific risks is vital. The erratic behavior you see after they've been drinking or the paranoia that skyrockets with stimulant use aren't just "bad choices." They are clinical events that demand an integrated treatment response.
To make this clearer, let's break down what someone thinks they're getting from a substance versus what's actually happening to them.
Impact of Common Substances on Schizophrenia Symptoms
This table directly compares the perceived short-term "benefits" of common substances with their real-world clinical harms for someone with schizophrenia.
| Substance | Perceived Short-Term 'Benefit' | Actual Clinical Risks & Long-Term Harms |
|---|---|---|
| Cannabis | A feeling of relaxation and a temporary drop in anxiety. | Worsened cognitive deficits, increased paranoia, triggering of psychosis, and a severe lack of motivation. |
| Alcohol | Short-term relief from anxiety and feeling less inhibited. | Deepened depression, impaired judgment, makes antipsychotic medication less effective, and carries a much higher suicide risk. |
| Stimulants | A temporary surge in energy, confidence, and mood. | Intense paranoia, severe hallucinations, increased agitation, and a high likelihood of hospitalization and relapse. |
Seeing these patterns is the first step. The next is finding specialized care that knows how to treat both the schizophrenia and the substance use disorder at the same time, because treating one without the other simply doesn't work.
If you're in Massachusetts and this sounds like what's happening with your loved one, don't wait for things to get worse. Call our team at (888) 388-8660 to talk about how integrated treatment can break the cycle.
The Power of Integrated Treatment for Dual Diagnosis
Trying to treat schizophrenia and substance use separately is a bit like fixing a car's engine and transmission in different shops on different days. It just doesn't work. Because the two issues are so deeply intertwined, this kind of fragmented approach rarely leads to lasting recovery. Real, sustainable healing from this dual diagnosis requires a unified strategy—and that's exactly why integrated treatment has become the gold standard of care.
This modern, more effective approach is a world away from the old, sequential models, where someone was often told, "Get sober first, then we'll deal with your mental health." This method almost always led to a frustrating cycle of relapse, since the untreated symptoms of schizophrenia would inevitably fuel the urge to use substances again. Integrated treatment shatters that cycle by embracing a simple truth: you can't heal one condition while ignoring the other.

What Integrated Care Looks Like
A truly integrated program is one where psychiatric and addiction specialists operate as a single, cohesive team. This collaboration ensures every single aspect of a person's care is coordinated.
For someone navigating schizophrenia substance use, this means a psychiatrist who specializes in dual diagnosis manages their antipsychotic medications while also considering treatments for addiction, like MAT (Medication-Assisted Treatment). At the same time, their therapist uses techniques like Cognitive Behavioral Therapy (CBT) to help them recognize and manage the overlapping triggers that spark both their symptoms and their cravings.
In an integrated setting, there is no "mental health team" and "addiction team." There is only the "recovery team," working from a single, shared treatment plan that honors the complexity of the individual's experience.
This approach creates a seamless safety net. Instead of trying to navigate two completely separate systems, individuals and their families here in Massachusetts can find all the care they need under one roof, guided by a team that's in constant communication.
Core Components of an Integrated Program
To be truly effective, an integrated treatment model must have several key components working in harmony. These elements ensure that both the psychiatric illness and the substance use disorder get the expert attention they need, at the same time.
- Unified Assessment: The journey begins with a comprehensive evaluation that looks at how the two conditions influence each other, rather than treating them as isolated problems.
- Coordinated Medication Management: A single prescriber oversees all medications. This is critical for maximizing benefits and, just as importantly, avoiding harmful interactions between antipsychotics and addiction-focused treatments.
- Dual-Focused Therapy: Therapy sessions—both individual and group—are specifically designed to tackle the unique challenges of a dual diagnosis, teaching coping skills for both psychosis and cravings.
- A Single Relapse Prevention Plan: Instead of two separate plans, clients create one cohesive strategy. This plan anticipates how mental health symptoms could trigger substance use, and how substance use could worsen symptoms.
By building a stable foundation for both conditions at once, this model gives people a much stronger shot at long-term recovery. For a deeper dive into this connection, you can learn more about how mental health and substance abuse are treated together in our specialized programs. True healing happens when care is comprehensive, coordinated, and compassionate.
Finding Integrated Treatment in Massachusetts
Knowing help is needed is the first, brave step. Actually finding that help is the next.
This is a practical guide for Massachusetts residents searching for specialized care when a loved one is battling both schizophrenia and substance use. It can feel like an impossible mountain to climb, but clear, effective, and compassionate support is closer than you might think.
We'll walk through the signs that professional help is non-negotiable and offer real advice on how to start that crucial conversation. At Paramount Recovery Centers, we are dedicated to breaking down barriers to care. That’s why we accept most major insurance plans and have a team ready to help you navigate your benefits, making the process feel accessible and achievable.
Recognizing When It's Time for Professional Help
It’s incredibly difficult to untangle the symptoms of schizophrenia from the effects of substance use. They often feed into each other, creating a confusing and chaotic picture.
However, certain patterns are red flags, signaling that the situation requires professional, integrated treatment. Recognizing these isn't about blame; it's about seeing the clinical reality of a dual diagnosis and understanding that it's far too much for anyone to handle alone.
Keep an eye out for these key indicators:
- Worsening Symptoms: A noticeable spike in psychotic symptoms like paranoia, hallucinations, or disorganized thinking, especially right after using drugs or alcohol.
- Treatment Non-Adherence: Constantly missing therapy appointments, refusing to take prescribed antipsychotic medications, or being unable to follow any part of a treatment plan.
- Social Isolation: Pulling away from family, friends, and things they used to love. This is often a way to hide the extent of their substance use.
- Increased Hospitalizations: A revolving door of psychiatric crises, ER visits, or inpatient stays that seems to line up with periods of heavy substance use.
The care gap for psychosis is alarmingly wide across the globe. Despite the immense need, only about 29% of people with psychosis receive specialist mental health care. This staggering statistic, which you can read more about here, highlights just how vital local, accessible centers in Massachusetts are—especially ones equipped to manage complex dual-diagnosis cases.
Your Local Path to Recovery in Southborough MA
Finding the right program makes all the difference. Here at Paramount Recovery Centers in Southborough, MA, we specialize in creating truly individualized plans for people facing the immense challenges of schizophrenia and substance use. We get that recovery isn't a one-size-fits-all journey, which is why we offer different levels of care to meet people exactly where they are.
Our core programs for dual diagnosis include:
- Day Treatment (PHP): This is our most intensive outpatient option. It provides a highly structured and supportive environment five days a week, serving as a critical step-down from inpatient care or a strong starting point for those who need significant support.
- Intensive Outpatient Program (IOP): Our IOP offers a more flexible but still structured approach, with programming for several hours a day, a few days a week. This allows clients to keep up with work, school, or family life while getting the dedicated clinical care they need.
At Paramount Recovery Centers, our philosophy is simple: treat the whole person, not just the symptoms. Our integrated team of psychiatric and addiction specialists works together under one roof to provide seamless, coordinated care for every client.
We offer comprehensive dual diagnosis treatment programs built from the ground up to address both conditions at the same time, giving our clients the strongest possible foundation for lasting wellness.
Frequently Asked Questions
When you're facing a dual diagnosis of schizophrenia and addiction, the questions can feel overwhelming and urgent. It’s a path that often feels isolating, but getting clear, accurate information is one of the most powerful things you can do to find your way forward.
Can substance use cause schizophrenia?
This is one of the first questions on everyone's mind. The short answer is no, substances don't cause schizophrenia out of the blue in someone who was never at risk. However, for someone who already has a genetic vulnerability, heavy substance use—particularly with high-potency cannabis—can be a powerful trigger that causes the first episode of the illness. For someone already diagnosed, substance use dramatically worsens symptoms, making integrated treatment for schizophrenia substance use essential.
How do I help a loved one who refuses treatment?
This is one of the most painful situations a family can endure. The key is to approach them with compassionate boundary-setting, not confrontation. Use "I" statements to express your concern about specific behaviors (e.g., "I get scared for your safety when you miss your medication"). Resources in Massachusetts like Community Reinforcement and Family Training (CRAFT) can teach effective strategies. Your goal isn't to force recovery, but to create an environment where choosing it becomes the most supported option.
What does dual diagnosis treatment involve?
Effective treatment involves an integrated team of mental health and addiction specialists working together. This includes coordinated medication management (using antipsychotics for schizophrenia and potentially MAT for addiction), dual-focused therapy like CBT to address overlapping triggers, and a unified relapse prevention plan. This comprehensive approach gives individuals the best chance at long-term stability.
Is dual diagnosis treatment in Massachusetts covered by insurance?
Yes, in most cases. Federal and state parity laws require most insurance plans in Massachusetts to cover mental health and substance use disorders just as they would any other medical condition. Paramount Recovery Centers is in-network with most major providers. Our team can provide a free, confidential insurance verification to explain your specific benefits and costs.
At Paramount Recovery Centers, we know just how immense the challenges of a dual diagnosis can be. Our integrated team is here to provide the compassionate, expert care your family needs to start healing. Don't wait to find help. Call us at (888) 388-8660 today or visit our website to learn more.



