Mental health struggles and substance use are often two sides of the same coin. When one is present, the other frequently follows, creating a complicated relationship where each condition can trigger or intensify the other. This guide will help you understand this connection, recognize the signs, and find effective dual diagnosis treatment in Massachusetts.
Key Takeaways
- Dual Diagnosis is Common: Mental health and substance use disorders often occur together, creating a cycle where one condition worsens the other. This is known as a co-occurring disorder or dual diagnosis.
- Integrated Treatment is Essential: The most effective approach is integrated care, which treats both the mental health condition and the substance use disorder simultaneously, rather than as separate issues.
- Help is Available in Massachusetts: There are specialized programs in Massachusetts that offer evidence-based therapies like CBT, EMDR, and MAT to help individuals break the cycle and achieve lasting recovery.
- Recovery is a Journey with Support: The path to healing involves structured care, family involvement, and a solid aftercare plan to ensure long-term stability and wellness.
The Tangled Link Between Mental Health and Substance Use
Think of two vines that have grown so tightly together you can't tell where one ends and the other begins. That’s a pretty good picture of how mental health and substance abuse are connected for so many people.

When these conditions exist together, they create a powerful cycle that can feel impossible to break without the right kind of specialized, integrated care.
This dynamic is what we in the field call a co-occurring disorder or dual diagnosis. It simply means someone is dealing with both a mental health challenge, like depression or anxiety, and a substance use disorder at the same time. Trying to fix just one part of the problem rarely works and often leads to a frustrating cycle of relapse and incomplete healing. Understanding this deep-rooted connection is the critical first step toward breaking free and finding lasting recovery right here in Massachusetts. You can read more about this troubling relationship between mental health and addiction in our detailed article.
A dual diagnosis isn't about having two separate problems; it's about having one complex condition where mental health and substance use are two sides of the same coin. True recovery means healing both sides at once.
The Vicious Cycle of Self-Medication and Dependency
When mental health issues and substance use get tangled up, they create a powerful, self-feeding loop. This isn't a simple case of one causing the other; it's a destructive dance where each condition makes the other worse, making it almost impossible to fix one without addressing its partner. Getting a handle on this cycle is the first real step toward breaking free.
The whole thing often starts with a search for relief. Someone drowning in the symptoms of an untreated mental health condition, like the constant hum of anxiety or the crushing weight of depression, might reach for a substance just to get a temporary break. This is what we call self-medication.
Using Substances to Cope with Symptoms
Think about a Massachusetts veteran struggling with PTSD. The intrusive memories and constant state of high alert turn everyday life into a minefield. Alcohol can feel like a way to turn down the volume and numb the pain, offering a brief moment of quiet.
Or consider a Boston college student with crippling social anxiety who uses marijuana before a party just to feel normal and outgoing. In that moment, the substance feels like the answer, but it's a short-term fix with a very high long-term cost.
The temporary escape offered by self-medication is a dangerous trap. While substances might briefly cover up the symptoms of a mental health condition, they do nothing to solve the root problem and almost always make it worse over time.
This coping strategy quickly spirals. The brain starts to link relief not with healthy skills, but with the substance. As tolerance builds, it takes more and more to get the same fleeting effect, paving a direct path to chemical dependency.

How Substance Use Worsens Mental Health
But the cycle isn't a one-way street. Heavy or long-term substance use physically changes the brain's chemistry, which can either kickstart a brand-new mental health disorder or pour gasoline on an existing one.
For example, alcohol is a depressant. Chronic use can throw the brain's natural mood-regulating chemicals out of whack, sometimes leading to a major depressive disorder. Stimulants like cocaine or meth can trigger intense anxiety, paranoia, and even psychosis by first flooding the brain with neurotransmitters and then causing a devastating crash. The link between dopamine and addiction is especially powerful here, as drugs hijack the brain's reward system, making it harder to feel pleasure from anything else. You can read more about this in our guide on how dopamine and addiction connect.
This creates a cruel feedback loop:
- A person feels depressed, so they drink to feel better.
- The alcohol makes their depression worse over time.
- They now feel an even stronger urge to drink to escape the deeper depression.
Shared Risk Factors and Vulnerability
Some people are more vulnerable to developing both a mental health and a substance use disorder from the start. Think of these shared risk factors like dry kindling, making it much easier for the fire of a co-occurring disorder to catch and spread.
Common vulnerabilities include:
- Genetics: If addiction or mental illness runs in your family, your predisposition to both can be higher.
- Environmental Stress: Growing up in a chaotic home, facing poverty, or living in a high-stress environment can lay the groundwork for both issues.
- Trauma: Experiencing physical, emotional, or sexual abuse is a massive risk factor. People often turn to substances to cope with the deep psychological wounds left behind.
For anyone caught in this cycle, the only way out is to treat both conditions with equal urgency. Trying to separate them is like fighting a fire by removing the fuel but ignoring the heat. Real, lasting recovery depends on an approach that heals the whole person. If you or a loved one in Massachusetts are struggling, call us at (888) 388-8660 for a confidential conversation about how to start healing.
Recognizing the Signs of Co-Occurring Disorders
When someone is dealing with both a mental health condition and a substance use issue, figuring out what's really going on can feel like trying to solve a puzzle with all the pieces jumbled together. The symptoms of one problem often mask or mimic the symptoms of the other. This messy overlap makes it incredibly hard for friends, family, and even the person struggling to see the whole picture.
This confusion is one of the defining features of co-occurring disorders. Learning to untangle the signs is the critical first step toward getting the right kind of help. When you can identify the warning signs, you gain the power to understand the situation and seek out effective, integrated treatment.
Common Behavioral Warning Signs
Often, the first thing you’ll notice is a major shift in a person's daily life and routines. Someone with a dual diagnosis might start to pull away from friends, family, and hobbies they used to love. This isn’t just about wanting more alone time; it’s a symptom that could be driven by depression, anxiety, or the need to hide their substance use.
Other behavioral red flags include:
- Neglecting Responsibilities: A sudden nosedive in performance at work or school, or an inability to keep up with basic household chores and personal hygiene.
- Risky Behaviors: Getting involved in dangerous situations like driving under the influence, having unsafe sex, or ending up in trouble with the law.
- Secretiveness and Dishonesty: Lying about where they’ve been, downplaying how much they’re using, or hiding substances are all common signs.
These behaviors often feed into a destructive cycle. The consequences—like losing a job or damaging a relationship—pile on more stress, which in turn fuels both the mental health struggles and the substance use.
Emotional and Physical Indicators
Beyond what you can see on the outside, the internal chaos of a co-occurring disorder shows up in some powerful emotional and physical ways. Sudden, dramatic mood swings are a classic indicator. One minute a person might be irritable and angry, and the next, they’re overcome with a deep sadness or hopelessness.
Physically, you might see changes in their appearance, like unexplained weight loss or gain, poor skin tone, or just looking exhausted all the time. Their sleep can become completely erratic—they might be sleeping way too much or battling insomnia night after night.
The real challenge here is that any of these signs could be blamed on either a mental health issue or substance abuse alone. When they show up together, it’s a strong signal that both issues are probably at play and need to be addressed at the same time.
This visual shows that powerful cycle where the stress from a mental health condition leads someone to self-medicate, which ultimately spirals into dependency.
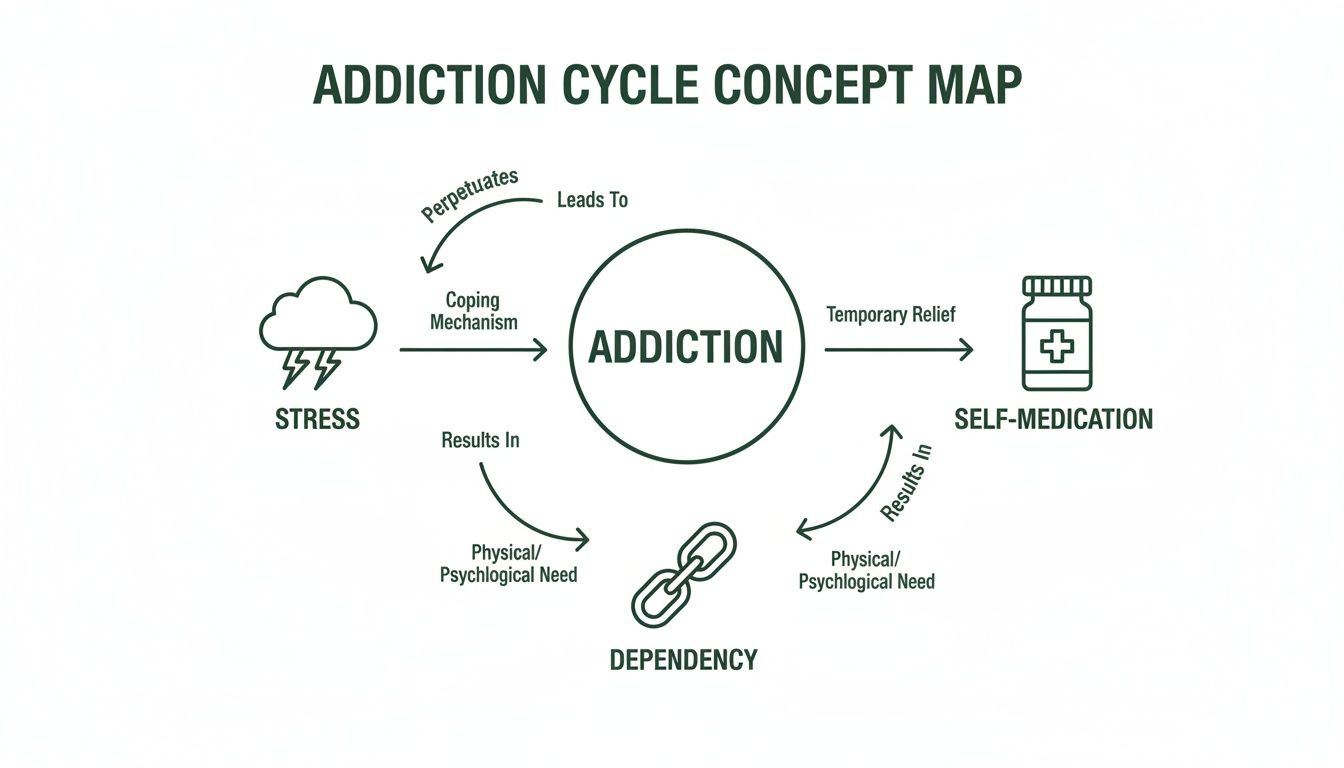
It’s a simple model that perfectly illustrates how a person gets trapped. The dependency itself creates even more stress, kicking off the loop all over again, often with greater intensity.
Spotting the Overlap in Symptoms
To cut through some of the confusion, it helps to see which symptoms are unique to one condition and which are shared between both. This table highlights some of the key distinctions that help clarify what a dual diagnosis can look like.
Comparing Symptoms in Mental Health vs Substance Use Disorders
| Symptom Area | Primarily Mental Health | Primarily Substance Use | Common Overlap (Dual Diagnosis) |
|---|---|---|---|
| Mood | Persistent sadness, loss of interest in hobbies (anhedonia). | Mood swings related directly to intoxication or withdrawal. | Extreme irritability, anxiety, feelings of hopelessness, anger. |
| Behavior | Social isolation due to depression or anxiety. | Developing a tolerance, experiencing withdrawal symptoms. | Neglecting responsibilities, sudden financial problems, secretiveness. |
| Cognition | Difficulty concentrating due to racing thoughts or apathy. | Impaired judgment specifically when under the influence. | Memory problems, trouble making decisions, poor focus. |
Recognizing these overlapping signs isn’t about making a diagnosis on your own. It's about realizing that a complex problem requires a specialized, expert solution. If you're seeing these patterns in yourself or a loved one in Massachusetts, it’s a clear sign that professional, integrated care is necessary.
The first step is making a confidential phone call. Contact our team 24/7 at (888) 388-8660 to talk about what you're seeing and learn more about the path forward.
Why Integrated Treatment Is the Gold Standard of Care
When you’re staring down both a mental health condition and a substance use disorder, trying to treat them separately is a recipe for failure. It’s like patching a hole in a boat but ignoring the crack right next to it—sooner or later, you’re going to sink. The old-school approach of sending someone to one facility for addiction and another for depression was clunky, disconnected, and just didn't work for most people.
Real, lasting recovery demands a smarter, more holistic strategy. That's where integrated treatment comes in. It's considered the gold standard because it addresses both issues together, at the same time, under one roof. This unified method acknowledges a fundamental truth: mental health and substance use are deeply tangled, and to heal one, you have to heal the other.

The Continuum of Integrated Care
Integrated treatment isn’t a one-size-fits-all program. Think of it as a journey with different levels of support tailored to where you are in your recovery. As you gain strength and stability, the intensity of care adjusts to match your progress. For those of us in Massachusetts, this path offers a clear, structured way forward, moving from stabilization toward a self-sufficient life.
This journey typically includes these key steps:
- Detox Placement and Coordination: For anyone physically dependent on a substance, this is the essential first step. It’s a safe, medically monitored space to manage withdrawal symptoms, clearing the way for the real therapeutic work to begin.
- Partial Hospitalization Program (PHP): Often called "day treatment," PHP offers the highest level of outpatient support. You'll engage in structured therapy for several hours a day, five days a week, while still living at home or in a sober living environment.
- Intensive Outpatient Program (IOP): This is the next step down. IOP provides robust clinical support but with a more flexible schedule, allowing you to gradually return to work, school, and daily life without losing your therapeutic safety net.
This step-by-step progression gives you the time and space to build new skills and confidence without feeling overwhelmed.
Evidence-Based Therapies That Heal Both Conditions
The real power of integrated treatment lies in using evidence-based therapies that are proven to work on co-occurring disorders. This isn't just about talking through your problems; it's about using targeted clinical tools to rewire destructive thought patterns, heal underlying trauma, and build healthy coping mechanisms. A good program will weave several of these approaches into a plan that's unique to you.
Some of the most effective therapies include:
- Cognitive Behavioral Therapy (CBT): CBT teaches you how to spot and challenge the negative thinking that drives both your mental health struggles and your substance use. It's like becoming a detective of your own mind, learning to intercept harmful thoughts before they spiral into harmful actions.
- Eye Movement Desensitization and Reprocessing (EMDR): When trauma is fueling the substance use, EMDR can be a game-changer. It helps the brain properly process and file away "stuck" traumatic memories, draining them of their emotional charge and reducing the impulse to self-medicate.
- Medication-Assisted Treatment (MAT): Combining FDA-approved medications with therapy, MAT helps stabilize the brain by reducing cravings and easing withdrawal. This creates the mental space needed to fully engage in and benefit from the deeper psychological work of recovery.
The substance use crisis in America is staggering. As of 2023, an estimated 48.5 million people aged 12 or older—that's 17.1% of the population—had a substance use disorder in the past year. This includes 7.5 million people battling both alcohol and drug use disorders at the same time. What's truly shocking is that only about 1 in 4 people (23.6%) who needed treatment in the U.S. actually got it, highlighting a massive care gap. These figures drive home why accessible, integrated programs are so vital for the residents of Massachusetts. You can find more details on these substance use statistics on TherapyRoute.com.
By weaving these specialized therapies together, integrated care provides the best possible chance to finally break the cycle and build a solid foundation for a fulfilling life in recovery.
Finding Dual Diagnosis Treatment in Massachusetts
Making that first move toward getting help is almost always the hardest part. If you’re a Massachusetts resident tangled in the grip of both mental health struggles and substance use, the whole process can feel impossibly heavy, clouded by fear and uncertainty. Think of this section as your practical guide—a roadmap to cut through the confusion and empower you to get the help you absolutely deserve.
We'll walk you through everything from making that first confidential phone call to knowing what to ask a treatment center. The path to a healthier, more fulfilling life isn't just a fantasy—it’s right there, within your reach. Your journey to healing can start today.

What to Expect From Your First Call
Picking up the phone to ask for help is a monumental act of courage. When you call our compassionate admissions team at (888) 388-8660, you’ll be met with understanding and respect, not judgment. We’ve been there.
That first conversation is completely confidential, and there are no strings attached. An admissions coordinator will simply listen to your story, conduct a brief and private pre-assessment to get a sense of your situation, and answer any questions you have about treatment for mental health and substance abuse.
Verifying Insurance and Finding the Right Fit
Worrying about how to pay for treatment should never stop someone from getting help. A key part of that initial call is verifying your insurance benefits. Our team will work directly with your provider to figure out your coverage and clearly explain any out-of-pocket costs, so you have a solid financial picture right from the start.
This step allows us to focus on what really matters: finding the right level of care for you. Everyone’s story is different, which is exactly why a one-size-fits-all program just doesn't cut it. Our entire focus is on building personalized care plans that are shaped by your specific needs, challenges, and goals.
The need for this kind of care is staggering. The World Health Organization reported in 2025 that over 1 billion people worldwide are living with mental health disorders. This statistic isn't just a number; it highlights the critical need for accessible, high-quality care right here at home. For families in Massachusetts, it underscores why proven services that treat both mental health and substance abuse are so essential to our community’s well-being. Learn more about these global mental health findings on WHO.int.
Your recovery journey is yours alone. A quality treatment program will honor your individuality by creating a personalized plan that addresses your specific mental health needs, substance use patterns, and life circumstances.
Finding the right program means asking the right questions. Don’t ever hesitate to ask about a center's treatment philosophy, the kinds of therapy they offer, and what a typical day actually looks like. You can discover more about the programs we offer at our Massachusetts mental health and addiction treatment centers to get a better feel for what a specialized, integrated approach involves.

Frequently Asked Questions
What is a co-occurring disorder?
A co-occurring disorder, often called a dual diagnosis, is when someone struggles with both a substance use disorder (like an addiction to alcohol or drugs) and a mental health disorder (like depression, anxiety, or PTSD) simultaneously.
Which condition should be treated first?
The gold standard is to treat both conditions at the same time with an integrated treatment plan. Tackling them one at a time often fails because the symptoms of one can easily trigger a relapse in the other.
How is dual diagnosis treatment different from standard rehab?
Standard rehab often focuses primarily on substance use. Dual diagnosis treatment is an integrated model that addresses both addiction and underlying mental health conditions simultaneously with a specialized clinical team. This whole-person approach leads to better long-term outcomes.
Can my family be involved in my treatment?
Absolutely. Effective treatment programs view family involvement as a crucial part of recovery. This often includes family therapy sessions and educational programs to heal relationships and build a strong support system for your return home.
What happens after I complete a treatment program?
Finishing a program is a major milestone, but not the end of the journey. A quality provider will give you a comprehensive aftercare plan. This roadmap for long-term recovery includes referrals to therapists, local Massachusetts support groups like AA or SMART Recovery, and ongoing alumni services to help you protect your progress.
The path to recovery from co-occurring mental health and substance use issues is within your reach. At Paramount Recovery Centers, our dedicated team is here to guide you every step of the way with compassionate, evidence-based care right here in Massachusetts. Don't wait another day to start your journey toward a healthier, more fulfilling life. Call us now for a free, confidential consultation at (888) 388-8660. We are available 24/7 to help.



