Deciding to stop drinking is a major step, and understanding what comes next is crucial for a safe journey to recovery. One of the biggest questions is often, “How long does alcohol withdrawal last?” While the most intense physical symptoms typically resolve within a week, the complete timeline can vary. This guide breaks down what to expect, from the first few hours to the longer-term healing process, offering clarity and support for those in Massachusetts and beyond.
Key Takeaways
- Acute withdrawal typically lasts 5-7 days. The most severe symptoms usually peak between 24 and 72 hours after the last drink.
- The timeline is not universal. How long alcohol withdrawal lasts depends on factors like your drinking history, overall health, and whether you have co-occurring conditions.
- Medical supervision is critical. Detoxing alone can be dangerous, with risks of severe complications like seizures and Delirium Tremens (DTs). Professional detox centers in Massachusetts provide a safe, medically managed environment.
- Recovery continues after detox. Post-Acute Withdrawal Syndrome (PAWS) can cause psychological symptoms like mood swings and sleep issues for months. Ongoing support is essential for long-term success.
Your Guide to the Alcohol Withdrawal Timeline
Facing alcohol withdrawal is intimidating, there’s no way around it. But knowing what to expect can give you a roadmap for the journey ahead. It’s a different experience for everyone, heavily shaped by things like your drinking history and your overall health. Still, there’s a general pattern that helps frame what’s coming.
To give you a clear snapshot, here are four essential things to know about the alcohol withdrawal timeline:
- Initial Onset: Symptoms usually start to creep in within 6 to 8 hours after your last drink. This first phase often brings on milder feelings of discomfort—think anxiety, headaches, and shaky hands as your body begins to notice the absence of alcohol.
- Peak Intensity: The toughest stretch for most people happens between 24 and 72 hours. This is when symptoms can become severe, and the risk of serious complications is at its highest. It’s the window where professional medical supervision is absolutely critical.
- Severe Complications: A small number of people may experience Delirium Tremens (DTs), a very serious condition that can show up 2 to 3 days into withdrawal. This is a medical emergency and requires immediate help.
- Lingering Symptoms: Even after the acute phase is over, you might not feel completely out of the woods. Some people deal with Post-Acute Withdrawal Syndrome (PAWS), where symptoms like mood swings and sleep problems can stick around for weeks or even months as your brain chemistry works to find its balance again.
The length of withdrawal is tied directly to how long alcohol stays in your system. For those of us in Massachusetts looking for help, understanding this timeline is a crucial part of preparing for a safe detox. With alcohol use on the rise, getting professional support has never been more important. You can learn more about how the body processes alcohol in our guide.
Getting through this period safely is what matters most. If you or someone you care about needs guidance, our team is here to talk 24/7. Call (888) 388-8660 for confidential support and to learn about treatment options that can work for you.
The Stages of Alcohol Withdrawal A Detailed Timeline
Figuring out how long alcohol withdrawal lasts is a lot easier when you see it as a series of stages. Picture a storm rolling in: you get the early warnings, then it builds to its most intense point before finally, gradually, clearing up. While this timeline isn’t set in stone for everyone, understanding the typical progression can make all the difference in preparing yourself or a loved one for the road ahead.
Each stage brings its own set of physical and psychological symptoms as the brain and body scramble to find balance without alcohol. The number one goal is getting through this process safely, especially for those in Massachusetts looking for a fresh start.
Stage 1: The First Signs
The first phase of withdrawal usually kicks in within 6 to 12 hours after the last drink. During this period, your central nervous system, which has been slowed down by alcohol, starts to rebound with a jolt. This sudden overactivity is what triggers the first wave of symptoms.
These early signs are almost always uncomfortable, but they’re typically the mildest part of the experience. Many people describe it as a brutal hangover paired with overwhelming anxiety.
Common symptoms you might notice in Stage 1 include:
- Shaky hands (tremors)
- Constant anxiety and nervousness
- Headaches
- Nausea and vomiting
- Insomnia or fitful sleep
- Heavy sweating
This infographic gives a solid visual of the typical withdrawal journey—when it starts, when it peaks, and how long it generally lasts.
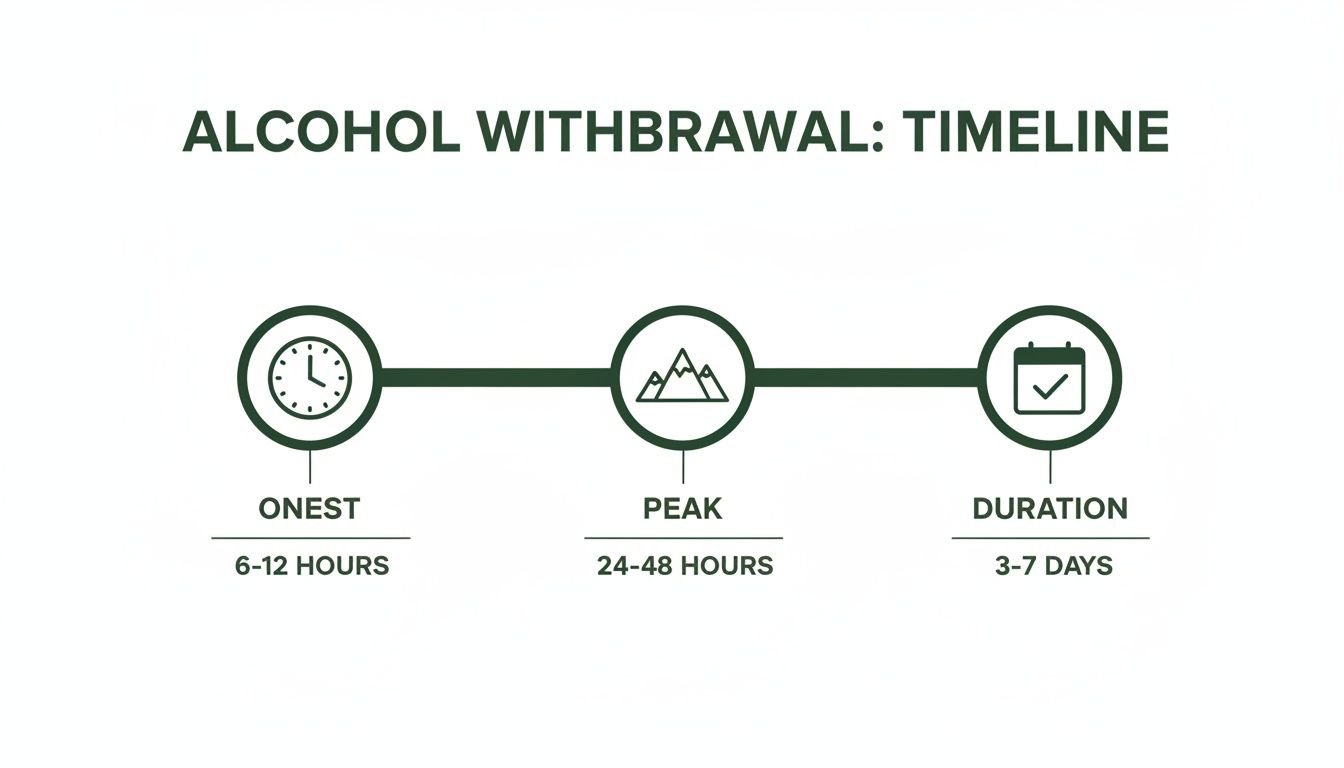
As you can see, things get started pretty quickly, but the real challenge builds over the next day or two.
Stage 2: Symptoms Escalate
Once you hit the 12 to 48-hour mark, the withdrawal storm really starts gathering strength. The early symptoms often get worse, and new, more alarming ones can surface. The nervous system’s hyperactivity ramps up, leading to greater physical and mental distress.
This is a critical window where medical supervision becomes incredibly important. It’s during Stage 2 that some people might experience alcoholic hallucinosis. Unlike the severe confusion seen later, individuals with these hallucinations are often aware that what they’re seeing or hearing isn’t really there.
Symptoms in this stage can feel completely overwhelming as the body and mind are under enormous strain. It’s a clear signal that the body is fighting hard to find equilibrium without alcohol’s dampening effects.
Here’s a quick look at what you can expect during the different stages of withdrawal.
Alcohol Withdrawal Timeline: What to Expect
| Stage | Time After Last Drink | Common Symptoms |
|---|---|---|
| Stage 1: Early Withdrawal | 6-12 Hours | Anxiety, insomnia, nausea, headache, shaky hands, sweating. |
| Stage 2: Escalation | 12-48 Hours | Increased heart rate & blood pressure, confusion, irritability, potential hallucinations. |
| Stage 3: Peak Symptoms | 48-72 Hours | High fever, severe agitation, vivid hallucinations, risk of seizures and Delirium Tremens (DTs). |
| Resolution | 3-7+ Days | Acute symptoms begin to fade, but psychological symptoms like anxiety and cravings may linger. |
This table provides a snapshot of the journey, but remember, everyone’s experience is unique.
Stage 3: The Peak and Risk of Severe Complications
The period between 48 and 72 hours is widely considered the peak of acute alcohol withdrawal. This is when symptoms hit their most severe point, and the risk for dangerous complications like seizures and Delirium Tremens (DTs) is at its highest.
During this stage, the body is in a state of extreme crisis. Seizures can happen suddenly, which is why a supervised medical detox center is the safest place to be. For a small number of people, usually those with a long history of heavy drinking, this is also when DTs can develop.
Key Symptoms at the Peak of Withdrawal:
- High Fever and Excessive Sweating: The body’s internal thermostat can go haywire.
- Severe Agitation and Confusion: Disorientation can become so intense that it’s hard to grasp what’s happening.
- Significant Tachycardia (Rapid Heart Rate): The heart is working overtime, putting cardiovascular health at risk.
- Vivid Hallucinations and Delusions: Unlike earlier hallucinations, the person may be convinced these experiences are real.
It’s vital to know that not everyone will go through these severe symptoms. But because the risk is so serious, trying to detox on your own is never a good idea. For a deeper dive, you can learn more about the specific alcohol withdrawal symptoms and what causes them.
After the 72-hour mark, the worst of the acute symptoms usually start to subside for most people. The storm begins to break, and the body can slowly start to heal. While the most immediate physical dangers may be passing, psychological symptoms and cravings can stick around for a while.
If you or someone you care about in Massachusetts is ready to stop drinking, understanding this timeline is a crucial first step toward a safe recovery. A professional medical detox program provides the support needed to manage these stages safely and as comfortably as possible.
Don’t wait for symptoms to become a crisis. Call us today at (888) 388-8660 for immediate, confidential guidance on starting your detox journey.
Understanding Delirium Tremens: The Most Severe Form of Withdrawal
While most people get through withdrawal with challenging but manageable symptoms, a small percentage will face something far more dangerous: Delirium Tremens (DTs). This isn’t just a ramped-up version of standard withdrawal; it’s a full-blown medical emergency that can be life-threatening and demands immediate professional care. DTs represents the absolute crisis point of the alcohol withdrawal timeline.
The reason we talk about DTs isn’t to scare you, but to drive home why a medically supervised detox is always the safest bet. Think of it like this: a bad cold is miserable, but you can usually handle it at home. Pneumonia, on the other hand, needs a doctor and serious medical treatment. DTs is the pneumonia of alcohol withdrawal—a profound state of confusion and physical crisis that is simply too dangerous to manage on your own.

What Separates DTs from Other Withdrawal Symptoms
The typical anxiety, shakes, and nausea of early withdrawal are a world away from Delirium Tremens. DTs involves a frightening shift in a person’s entire mental and physical state, signaling that the central nervous system is in total disarray. It most often kicks in 48 to 72 hours after the last drink, right when other withdrawal symptoms are hitting their peak.
The key signs that set DTs apart from less severe withdrawal are unmistakable:
- Profound Confusion and Disorientation: The person may have no idea who they are, where they are, or even what year it is.
- Vivid Hallucinations: These aren’t just seeing shadows in the corner of your eye. People with DTs can have powerful visual, auditory, or tactile hallucinations that feel completely real, leading to terror and agitation.
- Severe Autonomic Instability: The body’s core functions go haywire. This means dangerously high blood pressure, a racing heart, and a high fever.
- Grand Mal Seizures: These are severe, convulsive seizures that are a hallmark of the condition and can cause serious injury.
This combination of symptoms creates a perfect storm, making an unmonitored detox incredibly risky.
Who Is Most at Risk for Developing DTs?
Thankfully, Delirium Tremens is relatively rare. It’s not something that happens after one bad weekend of binge drinking. It’s almost always linked to a long history of chronic, heavy alcohol use.
The body becomes so dependent on the constant presence of alcohol that its sudden removal sends the entire nervous system into chaos. This is why individuals with years of heavy, daily drinking are the most vulnerable.
Other major risk factors include:
- A History of Previous Withdrawals: Every time someone goes through detox, their brain can become more sensitive—a process known as “kindling.” This increases the odds of more severe symptoms, including seizures and DTs, with each subsequent withdrawal.
- Co-Occurring Medical Conditions: Poor overall health, liver damage, or other chronic illnesses can make the body less able to cope with the immense stress of withdrawal.
- Older Age: The extreme physiological demands of DTs can be particularly dangerous for older adults.
Why Medical Supervision Is Non-Negotiable
The severity of DTs can’t be overstated. Research shows it typically peaks 48-72 hours after the last drink and can impact anywhere from 3-5% to 20% of patients, depending on how severe their alcohol dependence is. In the past, the mortality rate for untreated DTs was as high as 35%. With modern medical care, that figure has plummeted to 1-5%. You can discover more insights about these hospitalization trends and DTs risks in this detailed study.
For anyone in Massachusetts with a history of heavy drinking, this statistic alone highlights why professional help is so critical. Medical detox centers offer the 24/7 monitoring, specialized medications, and supportive care needed to navigate these symptoms safely and prevent a crisis.
If you are worried about your risk or a loved one’s, please don’t try to guess. Call our confidential helpline at (888) 388-8660 to talk to a specialist who can help you find the safest path to recovery.
What Is Post-Acute Withdrawal Syndrome (PAWS)?
Just when you think you’ve battled through the worst of withdrawal, you might find that the storm hasn’t completely passed. This lingering sense of unease, brain fog, and emotional turbulence is often Post-Acute Withdrawal Syndrome (PAWS), a very real, yet frequently misunderstood, part of long-term recovery.
It’s crucial to understand that PAWS is not a relapse or a sign that you’re failing. It’s your brain’s slow and steady process of healing after being dependent on alcohol for a long time.
Think of it like the aftershocks following a major earthquake. The main quake is over, but the ground remains unsettled for a while, with smaller tremors popping up unexpectedly. PAWS is a lot like that, causing unpredictable waves of symptoms long after the physical part of withdrawal is finished.
Why PAWS Happens and What to Expect
When someone is deep in active addiction, their brain chemistry changes to adapt to the constant presence of alcohol. Neurotransmitters like GABA and glutamate get thrown way out of balance. When you quit drinking, it takes a surprisingly long time for your brain to rewire itself and find its natural rhythm again. This slow recalibration is what causes PAWS.
Symptoms can show up without warning, often triggered by stress, and they look different for everyone. While the intense, acute phase of withdrawal is usually over in about a week, PAWS symptoms can linger for several months or, in some cases, up to a year or two.
Some of the most common signs of PAWS include:
- Mood Swings: Feeling irritable one moment, then anxious or depressed the next, with little warning.
- Sleep Issues: A frustrating inability to fall asleep, stay asleep, or experiencing unusually vivid dreams.
- Low Energy: A deep, persistent fatigue that rest doesn’t seem to fix.
- “Brain Fog”: Trouble concentrating, remembering things, or thinking clearly.
- High Sensitivity to Stress: Finding that everyday pressures feel overwhelming and are much harder to handle.
How to Get Through PAWS
Navigating PAWS is all about learning to ride the waves instead of fighting them. It’s a marathon, not a sprint, and it demands patience, self-compassion, and a solid plan for self-care, especially for those of us in recovery here in Massachusetts.
One of the most powerful things you can do is create a predictable daily routine. A simple, stable schedule helps regulate your body’s internal clock, which in turn can stabilize your mood and improve your sleep. This means getting up and going to bed around the same time, eating regular, balanced meals, and fitting in some gentle physical activity each day.
“Managing PAWS is less about fighting the symptoms and more about building a lifestyle that supports the brain’s natural healing process. Structure, support, and self-compassion are your most effective tools.”
Professional support is also a game-changer. Therapy, especially Cognitive Behavioral Therapy (CBT), can give you practical tools to identify your triggers and manage difficult emotions and cravings. Connecting with local Massachusetts support groups, like AA or SMART Recovery, surrounds you with people who truly get what you’re going through.
Don’t underestimate the power of mindfulness practices like meditation and deep breathing. These techniques teach you to observe your feelings without getting swept away by them, which can dial down the intensity of anxiety and emotional reactions. Think of them as small, daily exercises that strengthen your ability to stay grounded.
If you’re struggling with PAWS or any other part of your recovery, you absolutely do not have to do it alone. Call us at (888) 388-8660 to talk to someone who understands and can connect you with the right support and resources.
Finding Professional Detox Support in Massachusetts
Trying to get through alcohol withdrawal on your own isn’t just tough—it can be downright dangerous. The safest and smartest path forward involves professional medical supervision. In a detox setting, experts can manage your symptoms, head off serious complications, and give you the stable ground you need to start recovering. For anyone in Massachusetts, reaching out for that help is the single most important move you can make.
Professional detox is the gold standard for a reason. It’s designed to handle the physical and psychological storm of withdrawal in a controlled, supportive place. Think of it as the difference between weathering a hurricane in a tent versus a reinforced storm shelter. A medical team provides the structure and tools you need to get through it safely.

Why Medical Detox Is the Safest Option
Attempting to detox at home by going “cold turkey” leaves you completely exposed to the most severe withdrawal symptoms, like seizures and Delirium Tremens. In a professional facility, you get 24/7 medical oversight from clinicians who know exactly what to watch for. They’ll monitor your vitals, help manage your discomfort, and can step in immediately if a medical crisis starts to brew.
The primary goal of medical detox is stabilization. By managing the acute physical symptoms of withdrawal, we create a safe space where the real work of recovery can begin.
This constant supervision is often combined with medication-assisted treatment (MAT), which can make the whole process much more bearable. These medications are used to:
- Dial down the intensity of cravings
- Prevent dangerous seizures
- Ease anxiety and agitation
- Help stabilize your blood pressure and heart rate
Finally, a professional detox center offers a trigger-free environment. Getting away from the people, places, and daily stressors tied to drinking lets you focus entirely on getting well, without the constant threat of an early relapse.
Finding the Right Massachusetts Program for You
Here in Massachusetts, there are different levels of care available to meet you where you’re at. Figuring out your options is the key to finding the right fit for your specific needs.
- Inpatient Detox Centers: This is the highest and most intensive level of care. It’s strongly recommended for anyone with a history of heavy, long-term drinking or who has had complicated withdrawals in the past. You’ll live at the facility, getting round-the-clock medical care and support through the toughest part of withdrawal.
- Outpatient Programs: For those with milder dependence and a solid support system at home, outpatient detox can be a good choice. You go to scheduled appointments for medical check-ins and therapy but continue living at home. Just know that this route requires a serious amount of personal commitment.
The best choice depends on your drinking history, your overall health, and what your home life is like. A professional assessment can help point you toward the safest and most effective path. To get a better sense of what’s available locally, you can explore this guide on finding the right drug detox in MA.
Take the First Step Today
Knowing how long alcohol withdrawal lasts is only half the battle; knowing how to get through it safely is the other, more important half. You absolutely do not have to do this alone. The right support is available right here in Massachusetts to help you manage your symptoms and start building a healthier life.
If you’re ready to take back control, our compassionate team is here to help you understand your options and start your journey. Your call is always completely confidential, and there’s never any obligation.
Call us 24/7 at (888) 388-8660 for immediate, confidential help.
FAQs: How Long Does Alcohol Withdrawal Last?
Navigating alcohol withdrawal brings up many urgent questions. Getting clear, straightforward answers can reduce anxiety and help you prepare for the road ahead. Here are some of the most common questions people have about the withdrawal timeline and process.
Can alcohol withdrawal last for months?
While the most severe, acute phase of alcohol withdrawal is typically over within a week, some psychological symptoms can persist. This is known as Post-Acute Withdrawal Syndrome (PAWS), and it can last for several months to over a year. PAWS symptoms include mood swings, sleep disturbances, anxiety, and fatigue as your brain chemistry slowly returns to normal.
How do I know if my alcohol withdrawal is severe?
Severe alcohol withdrawal is marked by symptoms that go beyond typical anxiety and tremors. Warning signs include hallucinations (seeing or hearing things that aren’t there), high fever, severe confusion, and seizures. The most dangerous form is Delirium Tremens (DTs). If you experience any of these symptoms, it is a medical emergency requiring immediate attention. This is why detoxing under medical supervision in a Massachusetts facility is the safest option.

What helps with the anxiety from alcohol withdrawal?
Anxiety is one of the most common and difficult symptoms. In a professional detox setting, doctors may prescribe medications like benzodiazepines to calm the central nervous system and prevent more severe symptoms. At the same time, supportive care is crucial. Techniques like deep breathing exercises, mindfulness, and being in a calm, quiet environment can help manage anxiety. Staying hydrated and eating balanced meals also supports your body’s ability to cope.
When should I go to the hospital for alcohol withdrawal?
You should seek immediate medical help or go to the hospital if you experience any signs of severe withdrawal. These include seizures, hallucinations, extreme confusion or disorientation, a high fever, or a very rapid heartbeat. Because these symptoms can appear suddenly, the safest approach for anyone with a history of heavy drinking is to enter a professional medical detox program before symptoms have a chance to become a crisis.
At Paramount Recovery Centers, we know how overwhelming withdrawal can be, and we’re here to guide you through it safely. Our Massachusetts-based team offers personalized placement into detox and a full range of care to help you or your loved one start healing. You don’t have to do this alone. Call us 24/7 for a confidential conversation at (888) 388-8660.



